
Simplify your EHS tech stack
We offer the most comprehensive Environmental, Health, and Safety (EHS) management and compliance tools on the market that help you move the needle in your organization and allow you to invest in what matters most: your people.
Get startedA comprehensive EHS management system
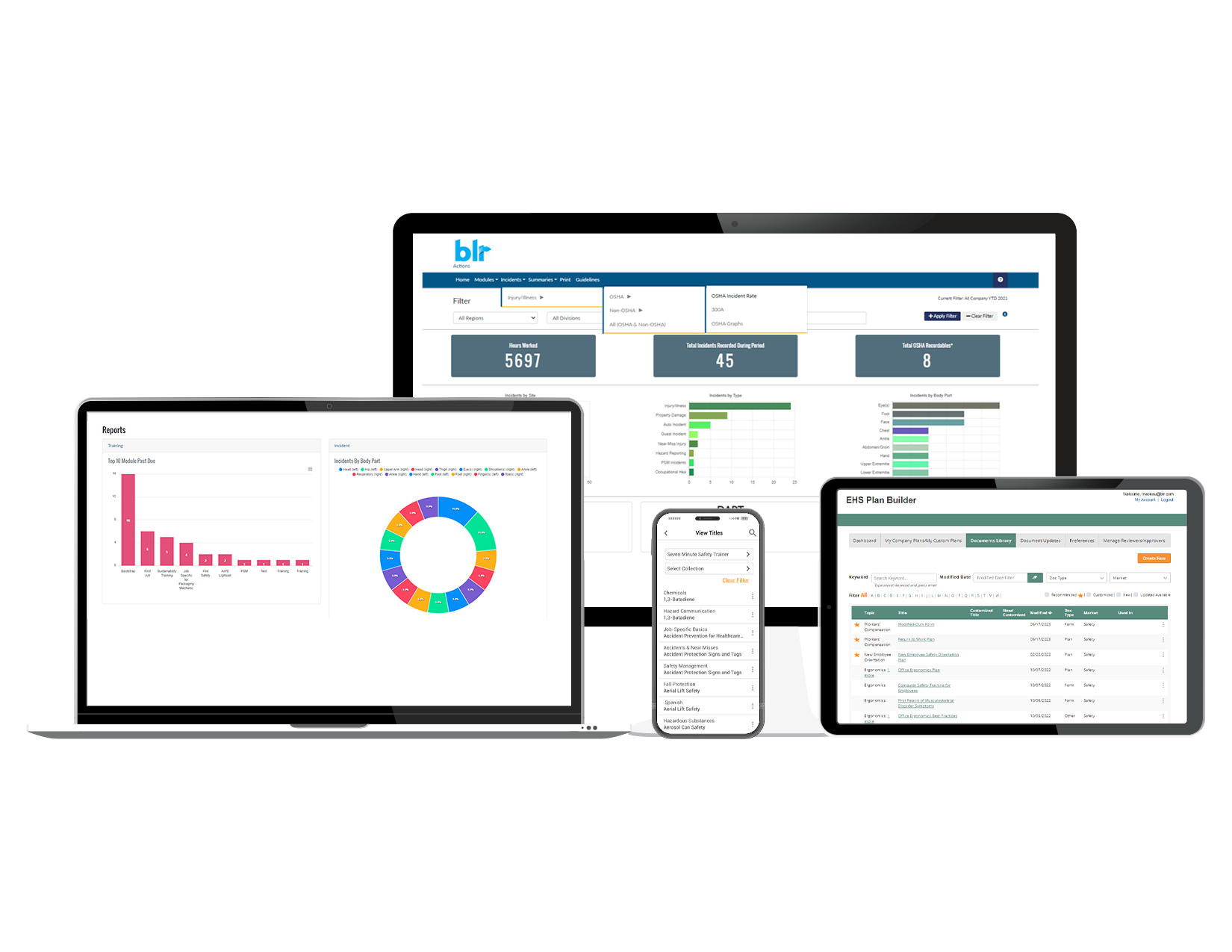
-
Regulatory compliance
Gain confidence that your organization complies with today’s regulations with actionable information.
-
Employee safety and engagement
Track all the incident types important to your company with our fully configurable incident management tool, which allows you to include injuries and illnesses, near-misses, environmental releases, and EHS activities for individuals involved with your organization..
-
Organizational efficiency and optimized workflows
Adjust EHS programs in real-time using leading and lagging indicators to ensure regulatory requirements are met and understood by key stakeholders.
-
Risk management
Quickly identify and assess potential risks in the workplace, develop measures to prevent and mitigate them, and establish a risk management plan.
Who benefits from EHS management?
EHS professionals, whether working individually or in teams, ensure environmentally responsible business practices and employee protection, adapting to evolving regulations. An adaptable and comprehensive EHS management system supports their integration with corporate sustainability and responsibility initiatives while staying up-to-date with industry changes for optimal performance.

-
Compliance management
We bring a collective 100+ years of experience investing over 50,000 hours annually to custom training development.
-
Incident management
Track all the incident types important to your company with our fully configurable incident management tool.
-
Risk management
Incorporate risk management into your EHS program with hazard assessments, risk analyses, and mitigation planning tools.
-
Training and education
Take advantage of the training and education tools to ensure your employees are informed on current regulations and practices.
An EHS system you can count on
Consisting of 28 tools, EHS Hero offers organizations powerful resources to help them manage their environmental, health, and safety programs more efficiently. With these tools, organizations can reduce risk, improve compliance, and create a safer and healthier workplace for their employees.
237 hrs
time saved annually streamlining critical compliance tasks
4.4
average client score from Capterra and G2
4.5x
average number of times EHS Hero subscribers have renewed
80%
of clients use EHS Hero every week
Annual hours saved
- 24 hrs saved permitting and recordkeeping
- 27 hrs saved on forms and checklists
- 54 hrs saved creating plans and procedures
- 48 hrs saved on training
- 84 hrs saved on regulatory research
Subject matter expertise
- Collective years of industry experience – 100+
- Hotline questions resolved – 4,200+
- EHS update newsletters deployed per year – 52
- Subject areas covered on EHS Hero – 197
Client insights
- On average EHS Hero subscribers have renewed 4.5 times
- 80% of people use EHS Hero every week
- 100% of EHS Hero subscribers say it helps them with regulatory research, training, or process automation.
- On G2 subscribers rank EHS Hero 4.3 out of 5 stars
- 41 industries served across current subscribers
- On Capterra subscribers rank EHS Hero 4.5 out of 5 stars
Tools and resources
- Mobile app tools – 9
- Mobile responsive tools – 20
- Training materials and modules – 4,000+
- Interpretations – 2,700+
- Guidance docs – 5,900+
- Forms – 6,700+
- Checklists – 600+
- Plans – 110+
- Toolbox Talks and micro training materials – 1,600+
EHS Solutions
Enhance your EHS program with our comprehensive solution of 28 tools, promoting a safer and healthier workplace for your employees.
Browse All Solutions-
Audits and Inspections
Allows for the building, completion, and tracking of any audit, inspection, survey or checklist.
Learn more -
Incident Reporting and Investigation
Keep track of all incidents and near misses and create OSHA 300 and 301 forms automatically.
Learn more -
Regulatory Analysis Chart Builder
Side-by-side comparison charts communicate what policies and practices must contain to avoid risk.
Learn more -
Process Safety Management
Compliance tracking with a built-in escalation process and automated reminders.
Learn more -
EHS Hotline
Receive plain-English answers to pressing questions from our subject matter experts and attorneys.
Learn more -
Plan Builder
Create custom plans that meet your organization's needs in minutes from a library of preloaded templates.
Learn more
Become an EHS hero
Featured resource
EHS Hero

